2023 U.S. Healthcare Projections (with help of ChatGPT® Part 3)
Healthcare Providers (primarily doctors, nurses, and clinicians) in the U.S. are in the middle of a crisis that is unprecedented in the last 50 years. This crisis has resulted from a veritable “perfect storm,’ events that have never manifested themselves simultaneously. The author, Nassim Nicholas Taleb would call it, a “Black Swan” – the result of rare events impossible to predict that can have a deep and lasting impact on individuals, businesses, and societies. I’d say that pretty well describes the COVID pandemic!
As we discussed in Part 2 of this series, post-COVID, costs have increased materially for all healthcare providers, while at the same time there has been a contraction and reduction of available healthcare personnel in all areas. The government and private insurance companies have FAILED to adjust for the increasing labor costs this has brought about. These are some of the conditions, along with runaway inflation throughout the economy, that we have not seen in the USA for more than 40 years. For 2023, Medicare actually cut cost for the basic reimbursement unit.
Though “physician services” are only about 15% of the National Healthcare Expenditures, they account for nearly authorizing all healthcare provided. No prescription can be issued without a doctor’s or trained clinician’s (ARNP, PA) signature (now 100% electronic), and no patient can be admitted or treated without a physician’s signature and supervision.
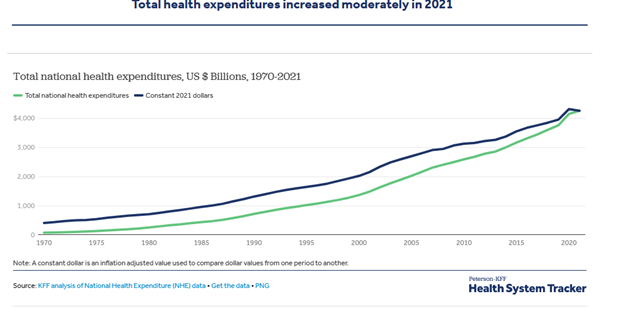
As we have witnessed, total healthcare costs have been consistently rising since 1960, and as reported by U.S. government data, U.S. “Physician and clinical services expenditures grew 5.6% to $864.6 billion in 2021”. Why is there a problem? Well, that data accounts for total gross payments, that are up, but a more accurate measure is the inflation adjusted per-encounter reimbursement which is down.
As an experiment, I asked ChatGPT® (more on ChatGPT in future blogs) to tell me “What are the financial and operational challenges faced by U.S. physicians in 2023?”, and it responded-
Financial Challenges:
One of the biggest financial challenges facing U.S. physicians is the decreasing reimbursement rates for healthcare services. Insurance companies are offering lower payments for services rendered, and this is putting a strain on the bottom line of many healthcare practices. Additionally, physicians are facing rising costs for malpractice insurance, employee benefits, and technology infrastructure.
Another financial challenge for physicians is the increasing administrative burden. Many physicians spend a significant amount of time dealing with paperwork and other administrative tasks, which takes time away from patient care and revenue-generating activities.
Operational Challenges:
Operational challenges facing U.S. physicians include the increasing demands for patient care and the shortage of qualified healthcare professionals. With the aging population, there is an increased demand for medical services, and physicians are struggling to keep up with the demand. Additionally, there is a shortage of qualified healthcare professionals, including nurses and medical assistants, which is putting a strain on physicians who are already stretched thin.
Another operational challenge facing physicians is the adoption of new technologies. Many physicians are hesitant to adopt new technologies, such as electronic health records and telemedicine, due to concerns about data privacy and security, as well as the cost and time involved in implementation.
Possible Solutions:
To address these financial and operational challenges, there are several possible solutions that physicians can consider. One solution is to collaborate with other healthcare providers, such as nurse practitioners and physician assistants, to provide a team-based approach to patient care. This can help to alleviate some of the workload and allow physicians to focus on higher-level tasks.
Another solution is to invest in new technologies that can help streamline administrative tasks and improve patient care. This may involve hiring additional staff or outsourcing administrative tasks to third-party providers.
Additionally, physicians can consider adopting value-based care models that focus on improving patient outcomes while also controlling costs. By aligning incentives around patient outcomes, healthcare providers can work collaboratively to deliver high-quality care while also controlling costs.Top of Form
I am stunned how well ChatGPT gets the problem with only the slightest prompt.
The reality, as someone that has been deep in healthcare from basic diagnostics to primary care, specialty care, healthcare technology, and even serving on the board of a medical school, the problems have never been worse and the potential for major improvement has never been better.
One of the biggest issues healthcare faces is that despite having tremendous diagnostic technology we have data everywhere; however, it’s not being used to even a fraction of its potential. This brings to mind the English poem that includes the line “water, water everywhere and not a drop to drink!” Today, this could translate to ‘data, data everywhere, but not a byte is useful!’ This directly translates to adversely affecting the physicians’ ability to provide both better care and lower cost.
Doctors and their staffs are working harder, yet more hours is not practical. As we have referred to in the past, this would be like using smaller needles to allow less painful “bloodletting” as in the 1800’s when we have much better tools that improve enable, and assist providers and improve the quality of care to their patients.
-Noel J. Guillama, Chairman

